

Understanding Neck Pain
Neck pain is common and can affect people of all ages. It may begin gradually after prolonged desk work, travel, or sustained screen use, or it can develop suddenly following an awkward movement, athletic strain, or trauma such as a motor vehicle collision. For some individuals, symptoms resolve quickly. For others, neck pain becomes recurrent, persistent, or associated with headaches, arm symptoms, or dizziness.
Although neck pain is often blamed on posture, arthritis, or disc problems, most cases are not the result of serious structural damage. Instead, symptoms usually reflect how the cervical spine is tolerating movement, sustained positions, and load, along with how the nervous system is responding to stress and previous injury.
Understanding the pattern of neck pain is more useful than focusing on a single structure or imaging finding. Different presentations respond to different strategies, and identifying the dominant pattern allows care to be specific and efficient.
If you are looking for detailed information about how neck pain is assessed and treated in our clinic, visit the Neck Pain Care page.
Why Neck Pain Happens
The cervical spine is designed to be mobile. It supports the head, allows rotation and visual tracking, and adapts continuously to changing loads throughout the day.
Neck pain often develops when the demands placed on this system exceed its current capacity. This may occur due to:
- Prolonged static postures
- Repetitive strain
- Sudden increases in training or workload
- Emotional or life stress
- Previous injury
- Trauma such as a fall or motor vehicle collision
Reduced cervical muscle endurance, particularly in the deep neck flexors and scapular stabilizers, can influence how well the neck tolerates sustained positions. When endurance is limited, even relatively low-level tasks such as desk work or driving can become provocative over time.
Prolonged screen use does not damage the spine. However, sustained positioning with limited movement variability can increase sensitivity in susceptible individuals.
After trauma, tissues may become irritated or sensitized. While most soft tissue injuries heal within weeks, ongoing symptoms may reflect persistent movement sensitivity or altered load tolerance rather than ongoing tissue damage. Imaging findings such as disc bulges or degenerative changes are common in people without symptoms, which is why clinical assessment remains more meaningful than scans alone.
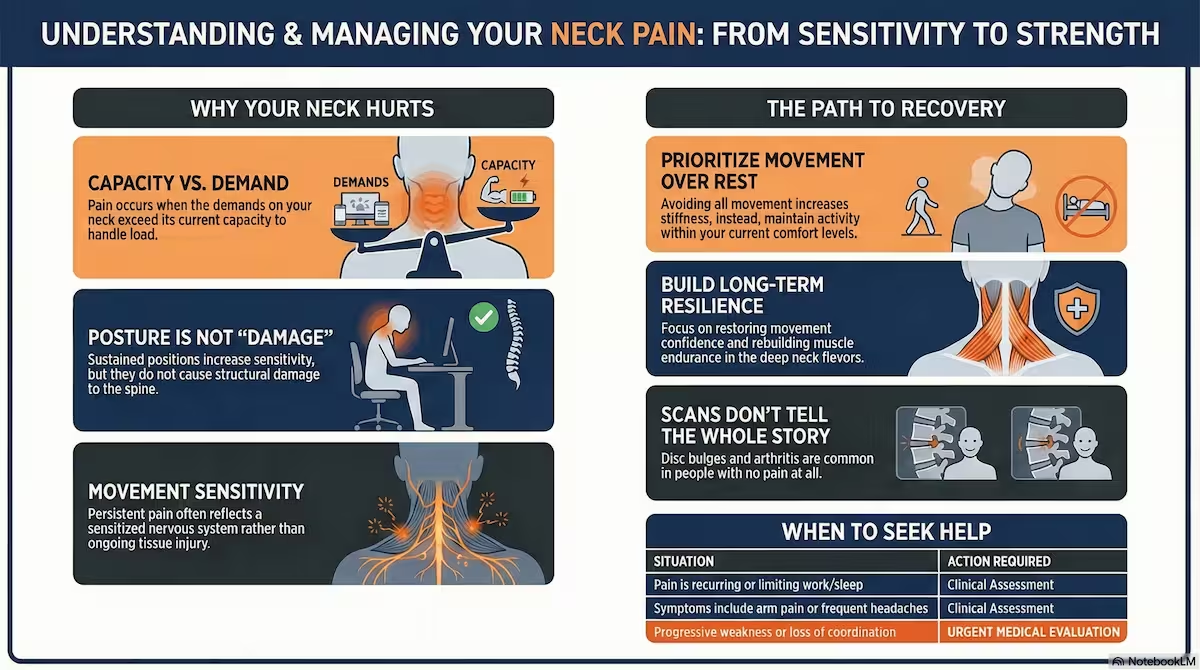
Common Patterns of Neck Pain
Not all neck pain behaves the same way. Recognizing the pattern helps guide management.
Mechanical or Movement-Related Neck Pain
This is the most common presentation. Symptoms often feel stiff, tight, or achy and are aggravated by prolonged sitting or sustained postures. Movement may feel restricted but typically improves with gentle mobility.
This pattern usually reflects reduced load tolerance rather than structural injury.
Disc-Related Neck Pain and Cervical Radiculopathy
Some individuals experience neck pain that worsens with prolonged flexion, such as looking down at a phone or computer. In certain cases, symptoms may extend into the shoulder or arm.
If a cervical nerve root becomes irritated, arm pain, tingling, numbness, or weakness may occur — a presentation often referred to as cervical radiculopathy.
For a more detailed explanation of this condition, see Cervical Radiculopathy.
Neck Pain and Headaches
Neck dysfunction can contribute to headaches, particularly when pain begins in the upper neck and radiates toward the head or behind the eye. These are commonly referred to as cervicogenic headaches.
They are often influenced by neck movement and sustained postures and may be accompanied by stiffness or restricted rotation. Identifying whether the cervical spine is contributing to headache symptoms is important, as management differs from primary migraine or tension-type headaches.
Learn more on our Cervicogenic Headache page.
Post-Traumatic Neck Pain (Whiplash)
Neck pain following a motor vehicle collision, fall, or sports injury may involve joint irritation, muscle guarding, and heightened nervous system sensitivity. While most soft tissue injuries improve within weeks, some individuals develop persistent pain driven more by altered load tolerance and movement sensitivity than ongoing tissue damage.
Early assessment and progressive loading are important to prevent symptoms from becoming prolonged.
For more information, see Whiplash and Post-Traumatic Neck Pain.
Neck Pain with Dizziness or Visual Sensitivity
Some individuals experience neck pain accompanied by dizziness, visual strain, or a sense of imbalance. This can occur following trauma or in persistent neck pain presentations.
The cervical spine contributes to balance and spatial awareness through interaction with visual and vestibular systems. When movement patterns are altered, symptoms such as lightheadedness or disequilibrium may develop.
Further detail is available on the Neck Pain and Dizziness page.
Persistent or Recurrent Neck Pain
For some individuals, neck pain becomes cyclical. Flare-ups may occur during periods of stress, increased workload, poor sleep, or prolonged inactivity.
Persistent symptoms often involve changes in movement confidence, endurance, and tissue sensitivity. A structured, progressive approach is typically required. Most mechanical and post-traumatic neck pain improves significantly with appropriate management.
When Is an Assessment Helpful?
Many episodes of neck pain improve within a few weeks, especially when movement is maintained and activity is gradually resumed.
An assessment may be helpful if:
- Pain is not clearly improving
- Symptoms are recurring
- Arm symptoms are present
- Headaches are frequent or worsening
- Movement feels restricted or guarded
- Pain is limiting work, sleep, or training
- Symptoms developed after trauma
Urgent medical evaluation is recommended if neck pain is accompanied by significant trauma with suspected fracture, unexplained weight loss or fever, progressive neurological deficits, difficulty with coordination or balance, or changes in bowel or bladder function. These presentations are uncommon but require prompt medical attention.
Next Steps
If you are experiencing back pain and are unsure which pattern fits, a structured assessment can help clarify what is driving your symptoms and what to do next.
Rather than focusing solely on imaging findings or temporary symptom relief, the goal is to understand how your back is functioning, what it is currently sensitive to, and how to improve its tolerance to movement and load.
A detailed evaluation looks at movement, strength, load response, and contributing lifestyle factors. From there, care can be tailored to the specific presentation — whether that involves movement modification, progressive loading, manual therapy, or a structured return-to-activity plan.
To learn more about how back pain is assessed and managed in our clinic, visit the Back Pain Care page.
How Neck Pain Is Managed
Management focuses on restoring movement confidence, rebuilding endurance, and improving load tolerance rather than relying solely on passive treatment.
Care may include:
- Targeted mobility work
- Progressive strengthening
- Manual therapy, like chiropractic care, when appropriate
- Education on load management
- Gradual return to work, sport, or training with the help of athletic therapy
The goal is not only symptom reduction, but improved resilience and reduced recurrence.
To understand our full assessment and treatment approach, visit the Neck Pain Care service page.
Related Conditions
Neck pain is often connected to related presentations. You may also find these pages helpful:
FAQ
Is neck pain usually serious?
Most neck pain is not serious and improves with time and appropriate movement. The majority of cases are mechanical in nature, meaning they relate to how the cervical spine is tolerating load and movement rather than structural damage. However, persistent symptoms, progressive neurological changes, or pain following significant trauma should be assessed.
How long does neck pain typically last?
Many episodes of neck pain improve within a few days to a few weeks. Post-traumatic or recurrent cases may take longer depending on irritability, load tolerance, and previous history. Most mechanical and post-traumatic neck pain improves significantly with appropriate management.
Can poor posture cause neck pain?
Sustained positioning with limited movement variability can increase sensitivity, especially if endurance is reduced. However, posture alone does not “damage” the neck. The issue is usually tolerance to sustained load rather than a single harmful posture.
What is cervical radiculopathy?
Cervical radiculopathy occurs when a nerve root in the neck becomes irritated or compressed. Symptoms may include neck pain with arm pain, tingling, numbness, or weakness. Most cases improve with conservative management, including guided movement and progressive loading.
Can neck problems cause headaches?
Yes. Dysfunction in the upper cervical spine can contribute to headaches, often called cervicogenic headaches. These headaches typically begin in the neck and radiate toward the head and may be influenced by neck movement or sustained positions.
Is imaging necessary for neck pain?
Imaging such as MRI or X-ray is not required in most cases of neck pain. Degenerative findings and disc changes are common in people without symptoms. Imaging is usually reserved for cases involving significant trauma, progressive neurological deficits, or when symptoms fail to improve as expected.
What should I avoid if I have neck pain?
Complete rest is usually not recommended. Avoiding all movement may increase stiffness and sensitivity. Instead, maintaining comfortable movement within tolerance and gradually rebuilding capacity is generally more helpful than immobilization.
When should I seek care for neck pain?
Consider an assessment if pain is not improving, symptoms are recurring, arm symptoms are present, headaches are worsening, or pain developed after trauma. Urgent medical attention is required if neck pain is accompanied by progressive weakness, coordination difficulty, loss of bowel or bladder control, unexplained fever, or significant trauma with suspected fracture.
Can neck pain cause dizziness?
In some cases, altered cervical joint function and movement patterns may contribute to dizziness or imbalance, particularly after trauma. However, dizziness can have many causes, so proper assessment is important to determine the source.
Does treatment only involve adjustments?
Management focuses on restoring movement confidence, rebuilding endurance, and improving load tolerance. While manual therapy may be used when appropriate, it is typically combined with progressive strengthening, mobility work, and education to improve long-term resilience.
What is vertebral subluxation, and does it cause neck pain?
The term vertebral subluxation has been used historically in chiropractic to describe a misalignment or dysfunction of a spinal segment believed to interfere with nerve function. In contemporary musculoskeletal research, there is limited high-quality evidence supporting the concept of a persistent spinal “misalignment” as a primary cause of most neck pain.
Modern understanding of neck pain emphasizes movement tolerance, tissue sensitivity, motor control, load management, and nervous system factors rather than fixed structural displacement. Imaging studies show that minor alignment variations are common in people with and without symptoms.
Current clinical guidelines for neck pain management focus on exercise, progressive loading, education, and, when appropriate, manual therapy — rather than correction of a static structural fault.
For readers interested in the historical and scientific discussion of the concept, see:
Bussières AE, Stewart G, Al-Zoubi F, et al. Spinal manipulative therapy and other conservative treatments for neck pain: clinical practice guideline. Journal of Manipulative and Physiological Therapeutics. 2016.
Bronfort G, Haas M, Evans R, Leininger B, Triano J. Effectiveness of manual therapies for the management of musculoskeletal disorders. Spine Journal. 2010.
Mirtz TA, Perle SM. The prevalence of the term subluxation in chiropractic degree program curricula throughout the world. Chiropractic & Manual Therapies. 2011.
